Spatio-temporal clustering of respiratory syncytial virus in Sakon Nakhon Province, Thailand, across the COVID-19 pandemic: A retrospective space–time scan analysis, 2019–2024
DOI:
https://doi.org/10.55674/cs.v18i2.265601Keywords:
Respiratory syncytial virus, RSV, spatio-temporal clusters, SaTScanAbstract
Respiratory syncytial virus (RSV) is a leading cause of acute respiratory infections in young children and older adults. The COVID-19 pandemic and the implementation of non-pharmaceutical interventions (NPIs) profoundly altered the transmission dynamics of RSV worldwide. However, evidence describing how RSV spatio-temporal patterns evolved across pandemic-related phases at fine geographic resolution remains limited in Thailand. We conducted a retrospective spatio-temporal cluster analysis of RSV cases reported in Sakon Nakhon Province, northeastern Thailand, between January 2019 and December 2024. Monthly RSV case counts from 125 sub-districts were analyzed using Kulldorff’s space–time scan statistic implemented in SaTScan, applying a space–time permutation model. The analysis was structured into three epidemiological phases: the pre-pandemic (January 2019–March 2020), NPI-associated suppression (April 2020–December 2021), and the post-pandemic resurgence (January 2022–December 2024). Nineteen space–time clusters were identified, eleven of which were statistically significant (p < 0.05). During the pre-pandemic phase, the primary cluster occurred between February 2019 and August 2020, encompassing nine sub-districts and exhibiting more than a sixfold excess of cases (relative risk [RR] = 6.08). Only one moderate-intensity cluster was detected during the suppression phase (RR = 2.71), reflecting markedly reduced RSV activity. Following relaxation of NPIs, RSV transmission rebounded sharply, with a large primary cluster between March and May 2022 involving 15 sub-districts and 1,059 cases (RR = 1.98), followed by multiple significant clusters persisting through 2024. RSV transmission in Sakon Nakhon Province showed marked spatio-temporal shifts across the COVID-19 pandemic, transitioning from localized pre-pandemic clustering to suppressed circulation during NPIs and subsequent widespread resurgence. These findings highlight the influence of pandemic-related interventions on RSV epidemiology and the importance of sub-district–level surveillance for preparedness and response in the post-pandemic era.
GRAPHICAL ABSTRACT
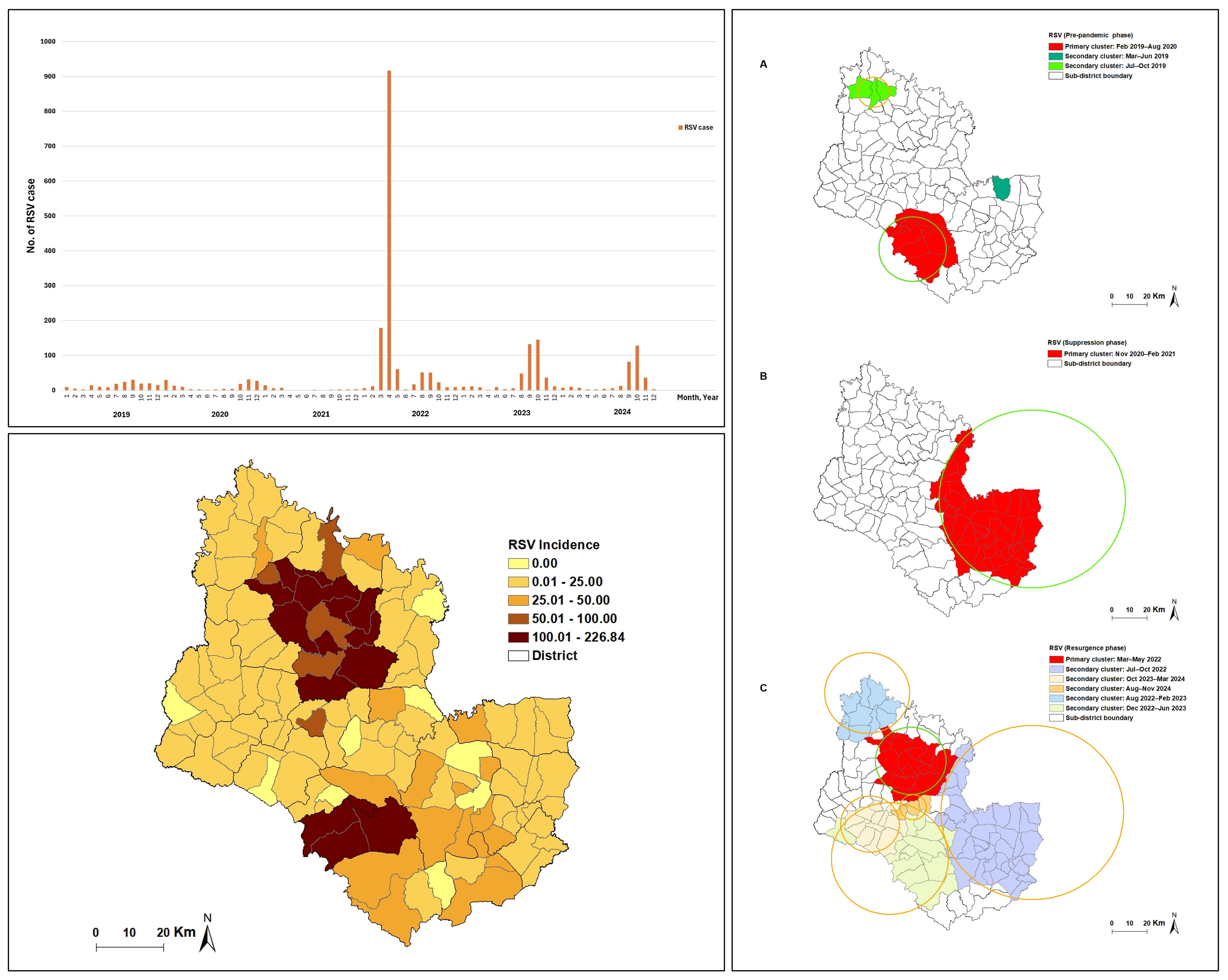
HIGHLIGHTS
- This study provides the first sub-district–level spatio-temporal analysis of RSV transmission in Thailand across the COVID-19 pandemic.
- Space–time scan statistics revealed a clear shift from localized pre-pandemic RSV clusters to widespread post-pandemic resurgence.
- RSV activity was markedly suppressed during COVID-19 non-pharmaceutical interventions, followed by atypical and prolonged outbreaks after restrictions were lifted.
- High-risk locations and outbreak windows were identified that were not apparent from province-wide surveillance alone.
- Fine-scale spatio-temporal methods offer actionable insights to strengthen early warning systems and hospital preparedness for RSV in the post-pandemic era.
References
Li, Y., Wang, X., Blau, D. M., Caballero, M. T., Feikin, D. R., Gill, C. J., Madhi, S. A., Omer, S. B., Simoes, E. A. F., Campbell, H., Pariente, A. B., Bardach, D., Bassat, Q., Casalegno, J. S., Chakhunashvili, G., Crawford, N., Danilenko, D., Do, L. A. H., Echavarria, M., …, Nair, H. (2022). Global, regional, and national disease burden estimates of acute lower respiratory infections due to respiratory syncytial virus in children younger than 5 years in 2019: A systematic analysis. The Lancet, 399(10340), 2047–2064.
Penders, Y., Brusselle, G., Falsey, A. R., Rohde, G., Betancur, E., Guardado, M. E., Agudelo, J. L. R., Saeedi, P., Harrington, L., & Michaud, J. P. (2025). Burden of respiratory syncytial virus disease in adults with asthma and chronic obstructive pulmonary disease: A systematic literature review. Current Allergy and Asthma Reports, 25(1), 14.
Brosh-Nissimov, T., Ostrovsky, D., Cahan, A., Maaravi, N., Leshin-Carmel, D., Burrack, N., Gorfinkel, R., & Nesher, L. (2024). Adult respiratory syncytial virus infection: Defining incidence, risk factors for hospitalization, and poor outcomes—A regional cohort study, 2016–2022. Pathogens, 13(9), 750.
Gamba-Sanchez, N., Rodriguez-Martinez, C. E., & Sossa-Briceno, M. P. (2016). Epidemic activity of respiratory syncytial virus is related to temperature and rainfall in equatorial tropical countries. Epidemiology and Infection, 144(10), 2057–2063.
Thongpan, I., Vongpunsawad, S., & Poovorawan, Y. (2020). Respiratory syncytial virus infection trend is associated with meteorological factors. Scientific Reports, 10(1), 10931.
Zheng, S., Zhou, W., Sun, Y., Lu, X., Song, S., Xie, X., Xiong, X., Zhang, H., Yuan, R., Zhang, Y., & Zhang, X. (2025). Impact of nonpharmaceutical interventions during the COVID-19 pandemic on the epidemiology and seasonal patterns of acute respiratory infections in children. Journal of Medical Virology, 97(8), e70522.
Principi, N., Autore, G., Ramundo, G., & Esposito, S. (2023). Epidemiology of respiratory infections during the COVID-19 pandemic. Viruses, 15(5), 1160.
Zhao, P., Zhang, Y., Wang, J., Li, Y., Wang, Y., Gao, Y., Zhao, M., Tan, H., Tie, Y., & Feng, Z. (2024). Epidemiology of respiratory pathogens in patients with acute respiratory infections during the COVID-19 pandemic and after easing of COVID-19 restrictions. Microbiology Spectrum, 12(11), e0116124.
Jiang, M. L., Xu, Y. P., Wu, H., Zhu, R. N., Sun, Y., Chen, D. M., Wang, F., Zhou, Y. T., Guo, Q., Wu, A., Qian, Y., Zhou, H. Y., & Zhao, L. Q. (2023). Changes in endemic patterns of respiratory syncytial virus infection in pediatric patients under the pressure of nonpharmaceutical interventions for COVID-19 in Beijing, China. Journal of Medical Virology, 95(1), e28411.
Chaiut, W., Sapbamrer, R., Dacha, S., Sudjaritruk, T., & Malasao, R. (2023). Epidemiology and associated factors for hospitalization related respiratory syncytial virus infection among children less than 5 years of age in Northern Thailand. Journal of Infection and Public Health, 16(10), 1659–1665.
Pasittungkul, S., Thongpan, I., Thongmee, T., Thatsanathorn, T., Poovorawan, Y., & Wanlapakorn, N. (2025). Longitudinal RSV antibody trends in Thai children (0–8 years): Association with seasonal outbreak patterns and potential immunity debt during the COVID-19 pandemic. Journal of Medical Virology, 97(10), e70629.
Thongpan, I., Vichaiwattana, P., Vongpunsawad, S., & Poovorawan, Y. (2021). Upsurge of human rhinovirus infection followed by a delayed seasonal respiratory syncytial virus infection in Thai children during the coronavirus pandemic. Influenza and Other Respiratory Viruses, 15(6), 711–720.
Sitthikarnkha, P., Uppala, R., Niamsanit, S., Sutra, S., Thepsuthammarat, K., Techasatian, L., Niyomkarn, W., & Teeratakulpisarn, J. (2022). Burden of respiratory syncytial virus–related acute lower respiratory tract infection in hospitalized Thai children: A 6-year national data analysis. Children, 9(12), 1990.
Kulldorff, M., Huang, L., Pickle, L., & Duczmal, L. (2006). An elliptic spatial scan statistic. Statistics in Medicine, 25(22), 3929–3943.
Kulldorff, M. (1997). A spatial scan statistic. Communications in Statistics – Theory and Methods, 26, 1481–1496.
Department of Provincial Administration, Ministry of Interior, Thailand. (2025, January 15). Official population statistics and administrative divisions of Sakon Nakhon Province. Department of Provincial Administration. https://stat.bora.dopa.go.th.
DIVA-GIS. (2025, January 20). DIVA-GIS. DIVA-GIS. https://www.diva-gis.org.
QGIS Development Team. (2025, 13 March). Quantum GIS (QGIS) version 3.40. QGIS. https://qgis.org/download.
Triukose, S., Nitinawarat, S., Satian, P., Somboonsavatdee, A., Chotikarn, P., Thammasanya, T., Wanlapakorn, N., Sudhinaraset, N., Boonyamalik, P., Kakhong, B., & Poovorawan, Y. (2021). Effects of public health interventions on the epidemiological spread during the first wave of the COVID-19 outbreak in Thailand. PLOS ONE, 16(2), e0246274.
Ndeh, N. T., Tesfaldet, Y. T., Budnard, J., & Chuaicharoen, P. (2022). The secondary outcome of public health measures amidst the COVID-19 pandemic in the spread of other respiratory infectious diseases in Thailand. Travel Medicine and Infectious Disease, 48, 102348.
Park, M., Choi, W. S., & Cowling, B. J. (2025). Shifts in influenza and respiratory syncytial virus infection patterns in Korea after the COVID-19 pandemic resulting from immunity debt: Retrospective observational study. JMIR Public Health and Surveillance, 11, e68058.
Holmdahl, I., Bents, S. J., Baker, R. E., Casalegno, J. S., Trovao, N. S., Park, S. W., Metcalf, J. E., Viboud, C., & Grenfell, B. (2024). Differential impact of COVID-19 non-pharmaceutical interventions on the epidemiological dynamics of respiratory syncytial virus subtypes A and B. Scientific Reports, 14(1), 14527.
Suntronwong, N., Vichaiwattana, P., Klinfueng, S., Korkong, S., Thongmee, T., Vongpunsawad, S., & Poovorawan, Y. (2020). Climate factors influence seasonal influenza activity in Bangkok, Thailand. PLOS ONE, 15(9), e0239729.
Srisingh, K., Khongthongprasert, S., Jaturabundit, T., Soponwaree, N., Klangsombat, K., Sriwad, C., Oilmungmool, N., Phuaksaman, C., & Lawanaskol, S. (2025). Risk factors for respiratory syncytial virus (RSV) infection in children under 5 years old with acute lower respiratory tract infection. Journal of Thoracic Disease, 17(7), 4565–4575.
Staadegaard, L., Caini, S., Wangchuk, S., Thapa, B., de Almeida, W. A. F., de Carvalho, F. C., Fasce, R. A., Bustos, P., Kyncl, J., Novakova, L., Caicedo, A. B., de Mora Coloma, D. J., Meijer, A., Hooiveld, M., Huang, Q. S., Wood, T., Guiomar, R., Rodrigues, A. P., Lee, V. J. M., … Paget, J. (2021). Defining the seasonality of respiratory syncytial virus around the world: National and subnational surveillance data from 12 countries. Influenza and Other Respiratory Viruses, 15(6), 732–741.
Ali, S. T., Tam, C. C., Cowling, B. J., Yeo, K. T., & Yung, C. F. (2020). Meteorological drivers of respiratory syncytial virus infections in Singapore. Scientific Reports, 10(1), 20469.
Zheng, Z., Pitzer, V. E., Warren, J. L., & Weinberger, D. M. (2021). Community factors associated with local epidemic timing of respiratory syncytial virus: A spatiotemporal modeling study. Science Advances, 7(26). eabd6421.
Olsen, S. J., Winn, A. K., Budd, A. P., Prill, M. M., Steel, J., Midgley, C. M., Kniss, K., Burns, E., Rowe, T., Foust, A., Jasso, G., Merced-Morales, A., Davis, C. T., Jang, Y., Jones, J., Daly, P., Gubareva, L., Barnes, J., Kondor, R., …, Silk, B. J. (2021). Changes in influenza and other respiratory virus activity during the COVID-19 pandemic—United States, 2020–2021. Morbidity and Mortality Weekly Report, 70(29), 1013–1019.
Yeoh, D., Foley, D., Minney-Smith, C., Martin, A., Mace, A., Sikazwe, C., Le, H., Levy, A., Blyth, C., & Moore, H. (2021). Impact of coronavirus disease 2019 public health measures on detections of influenza and respiratory syncytial virus in children during the 2020 Australian winter. Clinical Infectious Diseases, 72(12), 2199–2202.
Weinberger Opek, M., Yeshayahu, Y., Glatman-Freedman, A., Kaufman, Z., Sorek, N., & Brosh-Nissimov, T. (2021). Delayed respiratory syncytial virus epidemic in children after relaxation of COVID-19 physical distancing measures, Ashdod, Israel, 2021. Eurosurveillance, 26(29), 2100706.
Garg, I., Shekhar, R., Sheikh, A. B., & Pal, S. (2022). Impact of COVID-19 on the changing patterns of respiratory syncytial virus infections. Infectious Disease Reports, 14(4), 558–568.
Ujiie, M., Tsuzuki, S., Nakamoto, T., & Iwamoto, N. (2021). Resurgence of respiratory syncytial virus infections during COVID-19 pandemic, Tokyo, Japan. Emerging Infectious Diseases, 27(11), 2969–2970.
Foley, D. A., Yeoh, D. K., Minney-Smith, C. A., Martin, A. C., Mace, A. O., Sikazwe, C. T., Le, H., Levy, A., Moore, H. C., & Blyth, C. C. (2021). The interseasonal resurgence of respiratory syncytial virus in Australian children following the reduction of coronavirus disease 2019–related public health measures. Clinical Infectious Diseases, 73(9), e2829–e2830.
Lastrucci, V., Pacifici, M., Puglia, M., Alderotti, G., Berti, E., Del Riccio, M., Bonaccorsi, G., Moriondo, M., Resti, M., Peroni, D., Martini, M., Azzari, C., Gini, R., & Voller, F. (2024). Seasonality and severity of respiratory syncytial virus during the COVID-19 pandemic: A dynamic cohort study. International Journal of Infectious Diseases, 148, 107231.
Abu-Raya, B., Vineta Paramo, M., Reicherz, F., & Lavoie, P. M. (2023). Why has the epidemiology of RSV changed during the COVID-19 pandemic?. EClinicalMedicine, 61, 102089.
Zhang, S., Liang, H., Xu, J., Chen, B., Zheng, X., Lin, H., Wang, W., & Yao, Y. (2025). Spatial-temporal dynamics and virus interference of respiratory viruses: Insights from multi-pathogen surveillance in China. Journal of Infection, 91(2), 106556.
Fourgeaud, J., Toubiana, J., Chappuy, H., Delacourt, C., Moulin, F., Parize, P., Scemla, A., Abid, H., Leruez-Ville, M., & Frange, P. (2021). Impact of public health measures on the post-COVID-19 respiratory syncytial virus epidemics in France. European Journal of Clinical Microbiology & Infectious Diseases, 40(11), 2389–2395.
Razzini, J. L., Parada, D., Solovey, G., Guinazu, G., Sosa, E. M., Orta, S. R., Esposto, S., Fenelli, G. S., Regalado, A. E., Torre, V., Pichinenda, M., Ossorio, M. F., Souto, S. M., Ojeda, M. N., Lugo, S., Ferrero, F., Polack, F. P., Dvorkin, J., & Caballero, M. T. (2025). Impact and effectiveness of RSV maternal immunization on infant hospitalizations in Buenos Aires: A hospital-based, multicentre, retrospective surveillance cohort study. The Lancet Regional Health – Americas, 52, 101296.
Banooni, P., Gonik, B., Epalza, C., Reyes, O., Madhi, S. A., Gomez-Go, G. D., Zaman, K., Llapur, C. J., López-Medina, E., Stanley, T., Kantele, A., Huang, L. M., Mussi-Pinhata, M. M., Dewulf, J., Langley, J. M., Seidl, C., Ota, M., Kirabo, M., Anspach, B.,…., & Picciolato, M. (2025). Efficacy, immunogenicity, and safety of an investigational maternal respiratory syncytial virus prefusion F protein-based vaccine. Clinical Infectious Diseases, e146-e155.

Downloads
Published
How to Cite
Issue
Section
Categories
License
Copyright (c) 2026 Creative Science

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.










